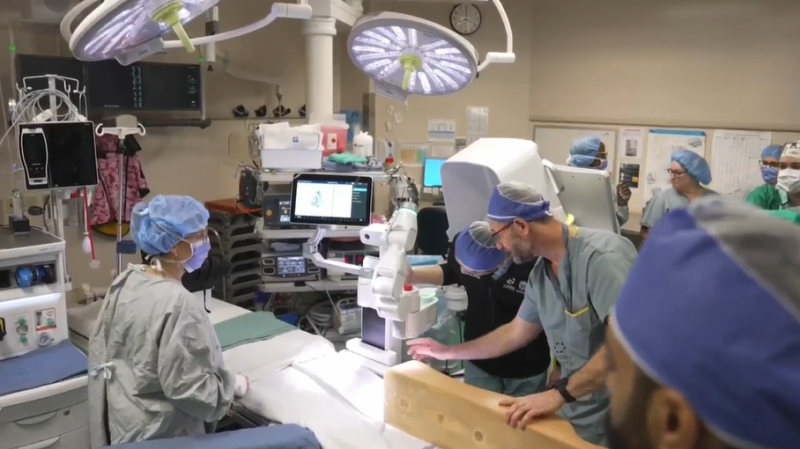
A London researcher is leading the way in using computers to help battle prostate cancer with a new software program he's developing.
Dr. Aaron Ward is designing a road map - a computerized, 3D road map - to help better diagnose and treat prostate cancer. And it's getting national attention.
On average, every day some 66 Canadian men are diagnosed with prostate cancer.
While it's one of the most common kinds of cancer, it's also one of the most curable, but the challenge is to find the right treatement.
"The issue is that prostate cancer takes on many forms...What this project that we're going to develop is about, it's about using Magnetic Resonance Imaging or MRI...to try to early and accurately determine which treatment is right for each patient."
A computerized road map uses artificial intelligence to help interpret the nuances in what's shown through an MRI.
Ward explains that the computer takes three different images of the prostate with different information, "and the idea is that this artificially intelligence system is going to automatically integrate and combine all of this information to produce a much simpler to read colour-coded road map for where the threatening areas of potential cancer are."
The expertise to read MRI images and translate them into effective treatment is typically concentrated in cities with major medical centres, like London, but the roadmap would extend this reach to other centres.
Ward says, "My hope is that this is going to enable widespread implementation of MRIs so that we can select the right treatment for each patient as they come in the door."
About $450,000 raised through the Movember campaign will be put toward the project through the Rising Star in Prostate Cancer Research grant.
And there's hope that down the road a prostate cancer road map could be a template for improvements in treating other cancers.
Ward explains, "Software is easy to translate, easy to implement. I'm not going to rest until we get this done, and I forsee that we can do this within the next five years."